ABSTRACT
The growing interest in Complementary and Alternative Medicine (CAM) and the increasing incorporation of its modalities in the United States’ healthcare system have exposed a number of problems in the field. These include a shortage of qualified CAM providers, scarcity of evidence-based research, lack of trained scientists in the field, and the ubiquitous marketing of frequently uncontrolled CAM products. Thus, the development of a comprehensive and scientifically sound educational infrastructure has become a crucial initial step in redirecting these adverse trends.
With support from the NIH-sponsored curricular CAM initiative, faculty from the department of physiology and biophysics at Georgetown University developed a M.S. program in CAM in 2003. This unique, first of its kind, science-based graduate program offers a master’s degree (MS) in physiology with an emphasis on CAM. The CAM-MS degree in physiology is designed to enable students to critically assess various CAM modalities, apply scientific rigor, and carry out evidence-based CAM research. The curriculum includes core science courses and CAM-related classes. Additionally, in order to emphasize the application of academic knowledge and further strengthen problem-solving skills, the students complete an eight-week summer practicum in a professional CAM-related environment.
Here, we report on our innovative and interdisciplinary CAM graduate program where creative teaching is implemented by basic scientists and enhanced by the application of their disciplines in tandem with the clinical expertise of CAM practitioners in the community. Thus, the faculty in the Department of Physiology & Biophysics is developing emerging cross disciplinary areas of study and interest in order to prepare new generations of future physicians, health professionals, educators, and researchers capable of objectively assessing the safety and efficacy of various CAM modalities, and introducing scientific rigor to much needed research into the various aspects of CAM therapies.
INTRODUCTION
Basic science departments are facing the continued challenge to maintain their identity and are in a constant state of defending their discipline and conserving graduation programs. However, in today’s era of interdisciplinary programs and translational research there may be other opportunities to use faculty expertise. The National Institutes of Health Road Map for Medical Research (http://nihroadmap.nih.gov/) delineated the importance of developing new innovative programs to promote an interdisciplinary workforce, thus encouraging the creation of interdisciplinary training programs at the undergraduate, graduate, and post-doctoral levels. In response to this call, a group of basic scientists at Georgetown University School of Medicine launched an educational initiative focused on incorporating Complementary and Alternative Medicine (CAM) material into the medical and graduate schools curricula. As a key component of this endeavor, a CAM Master’s of Science program in physiology was created and its first class enrolled in 2003.
Furthermore, it has been reported that medical students are eager to learn more about CAM during their academic training. As part of a broad survey conducted at six medical schools in the United States (Georgetown University), United Kingdom (two schools), Canada, Hong Kong, and New Zealand, the modified Integrated Medicine Attitude Questionnaire (IMAQ) was administered to first year medical students. Survey results indicated that 40.6% of students had previously used CAM, 22.5% had previously visited a CAM practitioner, and more interestingly, over two thirds (72%) expressed their eagerness to register in a special course on CAM.1 This trend did not change throughout their four years of training.2 Although from different cultural backgrounds, all students expressed interest in learning more about CAM. Moreover, voluntary participation in a survey by Georgetown University School of Medicine first and second year medical students revealed an overwhelmingly positive attitude towards CAM in general, personal use of CAM, experience with several CAM modalities, and a strong desire to acquire the knowledge base and training needed to effectively advise patients about CAM topics and refer them to CAM practitioners.3 In contrast, a survey of US medical schools teaching CAM revealed that only 17.8% of the schools focus on critical evaluation of the scientific literature, which should constitute the key instruction in assessing CAM efficacy and safety.4 These results clearly identify the need to incorporate CAM content into the curricula in order to enable the next generation of physicians and researchers to perform their duty in a responsible and competent manner.
The objective of this paper describes the development of an innovative program by basic science faculty that is anchored in multidisciplinary and collaborative academic activities. The primary focus of the CAM educational initiative is to train a new generation of students with a high level of CAM awareness and critical thinking. While some students’ interest is pursing a doctorate degree with an emphasis on translational research, most of the graduates are opting for careers as healthcare professionals.
Program Description
The goal of this program is to offer an academically rigorous graduate education in CAM embedded in biomedical sciences. The program is designed to be completed in 11 months with 30 credit hours, but additional options are available to students who would like to extend their studies over three semesters or enroll on a part-time basis. However, due to the scope and interactive nature of the program, neither evening classes nor long-distance web-based learning are available.
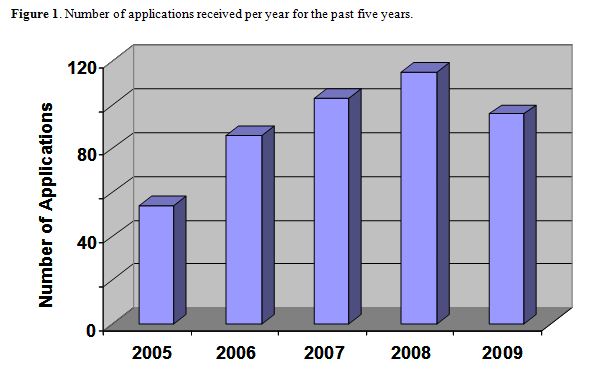
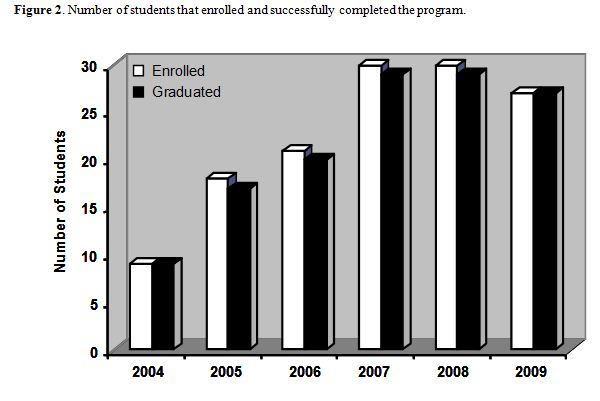
Applications and enrollment have tripled since the program’s inception in 2003 (Figure 1), and the number of students rose from 9 to 30. Due to the rapidly growing demand well beyond our current capacity, class sizes had to be capped at 25-30 students per year (Figure 2). To date, over 130 students joined our program and 98% have successfully completed the curriculum and graduated with a master’s of science degree in physiology with CAM emphasis.
In the fall of 2005, the basic science faculty expanded the program to include prospective Georgetown University School of Medicine medical students. Thus, a five-year MD/MS joint program based on the one-year CAM-MS program followed by the four-year medical school curriculum was launched. This combined program has generated unprecedented interest among medical school candidates, as demonstrated by enrollment.
Fall Semester
Students are required to take core courses in the conventional biomedical disciplines and CAM-based courses as well as select from a number of electives based on personal interest (Table 1). Fall semester courses include:
1) Cellular and Molecular Physiology, which covers many topics relevant to cellular physiology, such as cell signaling, glycolysis, and stress metabolism.
2) Introduction to Biostatistics, which is a basic statistics course conveying fundamental theory and application of biostatistics. A solid grasp of this subject is a pre-requisite in the field of biomedicine, as it constitutes the basis for sound scientific study design and analysis.
3) Survey of CAM course, wherein students are introduced to the five domains of CAM, as defined by the National Center of Complementary and Alternative Medicine, which include alternative medical systems, mind-body-medicine interventions, biology-based therapies, manipulation and body-based methods, and energy therapies. Lectures cover the modalities most commonly used in the United States, i.e., acupuncture, chiropractic care, massage therapy, naturopathy, homeopathy, Ayurveda, Unani, biofeedback, mind-body medicine, and energy therapies. These topics are complemented by student presentations and discussion sessions. Students are exposed to the theory and principles of these various CAM modalities and are trained to evaluate evidence (or lack thereof) of their efficacy and safety.
4) Conventional and Alternative Medicine in the USA: History of Conflicts and Commonalities was developed to provide historical and sociological perspectives of the changing relationship between alternative and conventional medicine in the United States. Understanding the eventful history of medicine and CAM is important in developing an objective opinion about medicine’s various schools of thought.
5) Mind-Body Skills was designed to promote effective stress management, self-awareness, and self-care among students. Didactic and experiential learning modalities are employed to teach eleven different mind-body-medicine techniques (meditation, imagery, biofeedback, autogenics).

6) Critical Readings in CAM is a course that provides the opportunity to analyze, critique, and discuss key scientific publications in the field of CAM.
Spring Semester
During the second semester, students are introduced to a new set of courses spanning both conventional and CAM fields. These courses include:
1) The Fundamentals of Human Physiology course covers the major areas of human physiology, including neurophysiology, cardiovascular, gastrointestinal, renal, and respiratory physiology, as well as endocrinology.
2) Physiologic Basis of Mind-Body Medicine addresses the involvement of the various psychoneuroimmulogic pathways in restoring balance and harmony and explores the physiology and mechanism of the mind-body medicine connection. The course complements the mind-body skills experiential component taught during the fall semester.
3) Herbal Medicine and Nutritional supplements offers an in-depth study of medicinal herbs, including their habitat, traditional use, current medical application, intentional or unintentional abuse, efficacy, and safety. Non-herbal dietary supplements are also covered in this course.
4) Human Nutrition and Health has been designed to emphasize the relationship between diet and health, and to introduce the concept of food as medicine.
Throughout the academic year, students attend the departmental Seminars in Physiology, Biophysics, and CAM, featuring invited speakers covering both conventional and CAM topics.
In addition, students have the choice of several CAM-related elective courses, such as Bioethics of Clinical Practice and Research in CAM, Western Practice of Eastern Medicine. In the former, basic ethical questions of “what treatments should be used, how should they be used,” and “in whom should they be used” are discussed in order to understand how these perspectives could contribute to the right and good conduct of patient care and research. The ethical obligations to conduct effective research are also highlighted. The latter, is an overview of Western medical research studies and ancient Eastern philosophical concepts that verify the importance of the link between mind and body. In conjunction with the Georgetown University Law School, students may opt for the Legal Aspects of CAM course as an elective. The course features current issues and challenges pertaining to accreditation, licensing, certification, scope of practice, and litigation occurring in the field of CAM, and participants have the opportunity to directly interact with lawyers and policy makers.
This innovative educational initiative fostered a cross talk among the different Georgetown University Schools and promoted collaborative activities with the practitioners in the community. They contribute valuable insights and medical practice-based information to this program. In addition, students have an opportunity to interact and build a network with healthcare providers in the community.
Summer Session
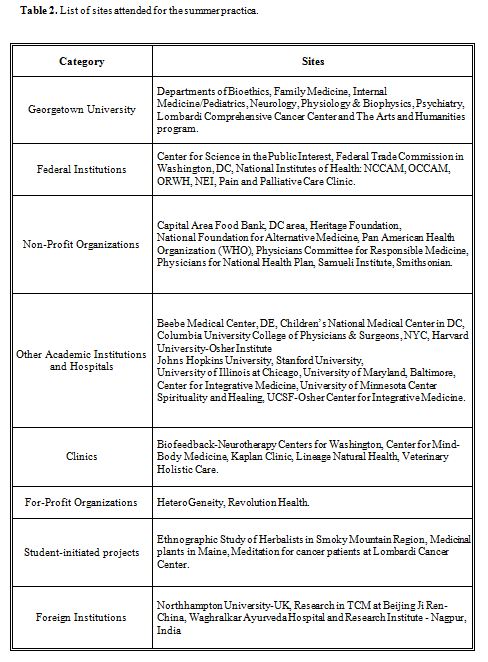
Students are required to conclude the academic year by completing an eight-week practicum at a CAM-related workplace. The environment should contribute to the student knowledge of CAM at the clinical, basic science, educational, regulatory affairs, and policy levels. Interactions with professionals offer students the opportunity to discuss relevant issues directly with experts in the field, and reinforce their classroom learning in a manner that may be useful in their future workplace or academic setting. The practicum also provides students with a network of relevant professional contacts.
Practica have been extremely diverse and included various positions at Georgetown University and other academic institutions throughout the US, federal agencies (NIH, Federal Trade Commission [FTC], and the Smithsonian Institution), and non-profit organizations (Center for Science in the Public Interest, National Women’s Health Network, Capitol Area Food Bank, Physicians for a National Health Program, and Physicians Committee for Responsible Medicine). Several students have worked at international agencies, including the Pan-American Health Organization (PAHO), and in clinical or laboratory settings in India, the United Kingdom, and the People’s Republic of China (Table 2).
Students
The CAM-MS Program in Physiology is a good educational experience for students interested in (i) medicine or healthcare-related professions who also seek a solid understanding of CAM, (ii) CAM-related basic science or clinical research that might extend to a doctoral level, (iii) administrative, legislative, policy or regulatory affairs careers, and (iv) CAM-related industry. During its past seven years, the program has attracted an ethnically diverse group from excellent academic institutions across the Nation. The program has also attracted international students and the enrollment has included students and two practicing clinicians from the American University of Beirut, University of Tokyo, United Kingdom, Turkey, China, Korea, Yemen, Ghana, Vietnam, and India.
The program graduates have pursued a variety of careers. While a majority of our graduates traditionally enter medical school, others have gone on to law school, or have pursued careers in dentistry, pharmacy, veterinary medicine, and acupuncture. With over 53% of our graduates in medical training, our program’s post-graduation placement rate is exceptionally high. In addition, over 30% of the program’s graduates are currently in the process of applying to medical school. Those who have directly entered the workforce are now working for federal agencies, industry, non-profit organizations, and some are teaching.
Our graduates are considered uniquely qualified for CAM–related positions and have continuously secured fellowships at NCI’s Office of Complementary and Alternative Medicine since 2005. Others are currently employed at the National Foundation for Alternative Medicine and the Samueli Institute (Figure 3).
The multi-disciplinary expertise of the faculty in the basic sciences, in healthcare, and in CAM was key to the launch and success of the program. Although, most faculty members are based in the Department of Physiology and Biophysics, additional faculty members from other departments and guest lecturers with exceptional skills and expertise participate in the teaching of our students and further contribute to the strength and uniqueness of this educational program.
DISCUSSION
The increasing proliferation of CAM practices is a global phenomenon that has not only been reported in the United States 5-6 but also in other countries, including the United Kingdom,7 France,8 Canada,9 and Turkey.10 The popular use of frequently unsubstantiated CAM therapies occurring in many parts of the world has lead to common concerns and calls for regulation. A nationwide survey conducted in Japan revealed a surprisingly high level of CAM use among cancer patients who had not consulted with their physicians.11 Similar results have been reported in surveys performed in Scandinavian countries. A nationwide survey in the United States revealed the use of CAM in combination with conventional medicine in the hope for better outcomes among 54.9% of the interviewed sample population, while 50.1% had tried CAM out of curiosity 6 ignoring the notion that CAM modalities are not necessarily safe, and that complications might occur due to drug-supplement and drug-herb interactions, or as a result of inappropriate treatment by unqualified practitioners. In a more recent survey, the authors also reported an increase in the use of acupuncture, deep breathing exercises and in and in meditation, massage, naturopathy, and yoga among adults between 2002-2007.12 The lack of reliable information regarding many CAM products and modalities combined with an insufficient CAM knowledge base leaves many physicians wondering about this emerging field. Inexperienced physicians hesitate to ask their patients about CAM, and patients frequently refrain from volunteering such information.13-15 In addition, healthcare providers lack a standardized method to effectively document CAM use in their patient histories.16 A recent study assessing physicians’ attitudes towards CAM revealed that 61% of physicians did not feel sufficiently knowledgeable in the field, and 81% voiced the desire to receive more CAM-specific education.17 In order to satisfy this growing need for evidence-based CAM information, and to support such information with scientific evidence, a creative model of CAM education and research based on modern technology and the scientific method has to emerge. In summary, Georgetown University’s CAM-MS Program in Physiology was created in response to (i) a nation-wide consumer-driven interest in CAM, (ii) the rapidly progressing clinical integration of various CAM modalities, and (iii) the resulting demand for well-informed and properly trained healthcare providers and scientists. The development of a scientifically rigorous educational program within this field is crucial in providing the much-needed evidence-based framework and the intellectual rigor that would allow such experts and practitioners to educate, treat effectively, and distinguish facts from fiction. As research priorities at many institutions, including NIH, increasingly shift towards interdisciplinary approaches, Georgetown University’s program demonstrates how faculty in basic science departments can create innovative platforms for graduate studies in emerging fields that can be solidly anchored in the scientific disciplines.
ACKNOWLEDGMENT
The authors express their gratitude to the Georgetown University core faculty members teaching in the CAM-Physiology Master’s Program (Drs. Adriane Fugh-Berman, Thomas Sherman, Michael Lumpkin, Mrs. Nancy Harazduk). The authors acknowledge the efforts of Dr. Adam Myers in helping launch the program and co-directing it from 2003-2006.
A special thank you goes to the many healthcare providers, from the greater Washington area, who have dedicated their time to this teaching endeavor; last but not least to all the past and future graduates who are making this program a success and materializing the Faculty’s efforts by taking the lead in different professional sectors.
This program was developed with support from the National Institutes of Health, National Center for Complementary and Alternative Medicine (R25-AT000419 to Aviad Haramati and KO7-AT001193 to Hakima Amri).
REFERENCES
- Schmidt, K., Rees, C., Greenfield, S., Wearn, A.M., Dennis, I., Patil, N.G., Amri, H., Boon, H. Multischool, international survey of medical students’ attitudes toward “holism”. Acad Med. 2005;80(10):955-963.
- Rees, C.E., Wearn, A.M., Dennis, I., Amri, H., Greenfield, S.M. Medical students’ attitudes to complementary and alternative medicine: further validation of the IMAQ and findings from an international longitudinal study. Med Teach. 2009;31(2):125-132.
- Chaterji, R., Tractenberg, R.E., Amri, H., Lumpkin, M., Amorosi, S.B., Haramati, A.. A large-sample survey of first- and second-year medical student attitudes toward complementary and alternative medicine in the curriculum and in practice. Altern Ther Health Med. 2007;13(1):30-35.
- Brokaw, J.J., Tunnicliff, G., Raess, B.U., Saxon, D.W. The teaching of complementary and alternative medicine in U.S. medical schools: a survey of course directors. Acad Med. 2002;77(9):876-881.
- Eisenberg, D.M., Kessler, R.C., Van Rompay, M.I., Kaptchuk, T.J., Wilkey, S.A., Appel, S., Davis, R.B. Perceptions about complementary therapies relative to conventional therapies among adults who use both: results from a national survey. Ann Intern Med. 2001;135(5):344-351.
- Barnes, P.M., Powell-Griner, E., McFann, K., Nahin, R.L. Complementary and alternative medicine use among adults: United States, 2002. Adv Data. 2004(343):1-19.
- Wye, L., Sharp, D., Shaw, A. The impact of NHS based primary care complementary therapy services on health outcomes and NHS costs: a review of service audits and evaluations. BMC Complement Altern Med. 2009;9:5.
- Cottencin, A., Mullet, E., Sorum, P.C. Consulting a complementary and alternative medical practitioner: a systematic inventory of motives among French patients. J Altern Complement Med. 2006;12(8):791-798.
- Quan, H., Lai, D., Johnson, D., Verhoef, M., Musto, R. Complementary and alternative medicine use among Chinese and white Canadians. Can Fam Physician. 2008;54(11):1563-1569.
- Ozturk, C., Karayagiz, G.. Exploration of the use of complementary and alternative medicine among Turkish children. J Clin Nurs. 2008;17(19):2558-2564.
- Hyodo, I., Amano, N., Eguchi, K.,Narabayashi, M., Imanishi, J., Hirai, M., Nakano, T., Takashima, S. Nationwide survey on complementary and alternative medicine in cancer patients in Japan. J Clin Oncol. 20 2005;23(12):2645-2654.
- Barnes, P.M., Bloom, B., Nahin, R.L. Complementary and alternative medicine use among adults and children: United States, 2007. Natl Health Stat Report. 10 2009(12):1-23.
- Chao, M.T., Wade, C., Kronenberg, F. Disclosure of complementary and alternative medicine to conventional medical providers: variation by race/ethnicity and type of CAM. J Natl Med Assoc. 2008;100(11):1341-1349.
- Zhang, Y., Jones, B., Ragain, M., Spalding, M., Mannschreck, D., Young, R. Complementary and alternative medicine use among primary care patients in west Texas. South Med J. 2008;101(12):1232-1237.
- Frenkel, M., Ben-Arye, E., Hermoni, D. An approach to educating family practice residents and family physicians about complementary and alternative medicine. Complement Ther Med. 2004;12(2-3):118-125.
- Cockayne, N.L., Duguid, M., Shenfield, G.M. Health professionals rarely record history of complementary and alternative medicines. Br J Clin Pharmacol. 2005;59(2):254-258.
- Milden, S.P., Stokols, D. Physicians’ attitudes and practices regarding complementary and alternative medicine. Behav Med. 2004;30(2):73-82.