ABSTRACT
Methamphetamine abuse is a significant medical problem in our region. We developed and investigated an interclerkship curriculum to educate medical students about the significance of methamphetamine abuse and dependence and its effects on the individual and society. Topics covered include neuropathology, neuropharmacology, diagnosis, treatment, law enforcement issues and social services.
The primary care physician plays an important role in the identification of substance use in adolescents and adults.1 Approximately 20% of patients seeing a family physician have substance abuse problems.2 Physicians in training must understand they will see patients who suffer from substance abuse and dependence. They need to learn to recognize the red flags in the patient history, as well as specific physical findings related to substance use.2 Even though primary care physicians could treat substance abuse problems in their clinical setting, it is often prudent to refer patients to consultants who specialize in substance use disorders. Primary care physicians should know the appropriate resources in their region to facilitate appropriate referrals.
In 2007, Creighton University School of Medicine was named by the National Institute on Drug Abuse (NIDA) as one of four Centers of Excellence (COE) for Physician Information. The Centers of Excellence were established to serve as national models for the advancement of addiction awareness, prevention and treatment in primary care practices. Each NIDA COE identified drug addiction knowledge gaps and developed educational materials for physicians in training to address these gaps. Curricular materials were developed to provide information about methamphetamine abuse. Methamphetamine was chosen because it remains a serious problem in many Midwestern states, including Iowa, Minnesota, Montana, North Dakota and Nebraska, where our medical school is located. The production, transportation, distribution, and abuse of methamphetamine pose significant challenges for law enforcement and healthcare providers.
We developed a specialized, interclerkship module curriculum on methamphetamine. Interclerkship experiences, sometimes called intersessions, are employed by medical schools to address topics that are not emphasized in clinical clerkships but are relevant to clinical learners.3 Some schools have developed interclerkship experiences to provide students with information about emerging issues, such as bioterrorism, while other interclerkships are designed to address core content such as professionalism and evidence-based medicine.4–9 At least one interclerkship experience was developed to assess medical student attitudes toward and knowledge about substance abuse disorders and their confidence in conducting substance abuse assessment and intervention.10 These focused curricula are typically offered between clinical clerkships and use small group and other interactive learning methods.
The goal of this interclerkship module is to educate medical students about the significance of methamphetamine abuse and dependence, its effects on the individual and society and its treatment. Although designed for third-year medical students, the curriculum could be adapted for other medical students or residents. The learning objectives address 1) prevalence data on methamphetamine abuse and dependence, 2) diagnostic information, 3) neuropathology and neuropharmacology, 4) treatment options and goals, 5) educational resources and 6) local resources for the treatment of methamphetamine abuse and dependence.
The methamphetamine interclerkship module was introduced as part of the interclerkship course, Dimensions of Clinical Medicine (DCM), in 2008–2009. This course was introduced in 2002–2003, and has proven effective for presenting clinically relevant content to third-year students.11 Consistent with adult learning principles, the course offers students knowledge and skills at the time they are most likely to need them, i.e., during their first clinical year.12 Other course module topics include legal issues, palliative care, alternative medicine, substance abuse and human sexuality. The common thread is that these topics represent important competency areas, but are unlikely to receive adequate coverage in clerkships.
Interclerkship course modules occur bi-monthly, are composed of two half-day sessions or a one-day session and are mandatory. The modules employ multiple instructional methods, including lectures, small groups, panel discussions, and other interactive activities designed to promote student engagement and a cooperative learning environment. The school’s Educational Policy Committee appoints the course director for the entire DCM course, and the course director recruits course directors for each module. The course director for the methamphetamine interclerkship experience is a faculty member in the Department of Family Medicine who has interest and expertise in substance use disorders and treatment issues.
Although the course directors decided to introduce the methamphetamine interclerkship curriculum as a single half-day module, it could be offered as a one-day (8 hours) course or two half-day (4 hours) courses. The curriculum was developed to fit the Dimensions of Clinical Medicine course format, and was designed to promote active learning. The course directors for both the methamphetamine interclerkship module and Dimensions of Clinical Medicine course developed the course content, using NIDA resources. Feedback obtained from students after the pilot implementation will be used to revise the curriculum.
The methamphetamine module includes lectures on the diagnosis and treatment of methamphetamine abuse and dependence, law enforcement aspects of methamphetamine abuse and the neuropathology and neuropharmacology of methamphetamine abuse and dependence. The curriculum also features video clips from the NIDA/HBO production “Addiction” and a facilitated panel discussion with community members such as methamphetamine dependent individuals in treatment, social workers, community agency representatives and treatment professionals. Options for breakout sessions include a training session for diagnosing methamphetamine dependence with standardized patients, meeting with individuals recovering from methamphetamine dependence (consenting volunteers in recovery) and an introductory training session for motivational enhancement therapy (MET). The course ends with a debriefing and learning assessment. Sample course schedules for both 4- and 8-hour periods are presented in Table 1.
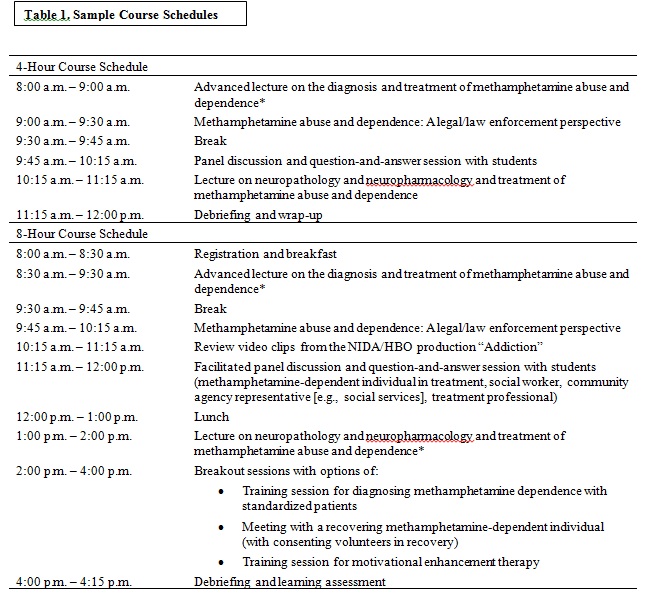
*The lecture slide presentation was developed by the module director. Content for the slide presentation was compiled primarily from NIDA resources. The slide set will be available to the public along with a companion lecture guide when Center of Excellence work is completed.
One hundred sixteen third-year medical students completed the methamphetamine interclerkship module––59 males (50.9%) and 57 females (49.1%). The directors of the methamphetamine interclerkship module and Dimensions of Clinical Medicine course are faculty in the departments of Family Medicine and Internal Medicine, respectively. Presenters from outside the university (e.g., law enforcement representative, attorney, and social worker) were invited by the course directors. The course directors oriented the presenters to the course goals and objectives before the session.
To evaluate the pilot implementation of the methamphetamine interclerkship module both quantitative and qualitative data were collected. Two instruments, a standard course evaluation and a brief learning assessment, were developed to assess student satisfaction and course impact. Both were administered at the conclusion of the course (Time 1) and six months later (Time 2). The program evaluation asked students to rate items on a Likert-style scale of 1 (strongly disagree) to 5 (strongly agree) and contained general items used in other interclerkship evaluations as well as items specific to the methamphetamine component. The program evaluation was available online immediately following the module. Six months afterwards, an abbreviated program evaluation was distributed electronically. The program evaluation results for Time 1 and Time 2 are reported in Table 2.
Table2. Program Evaluation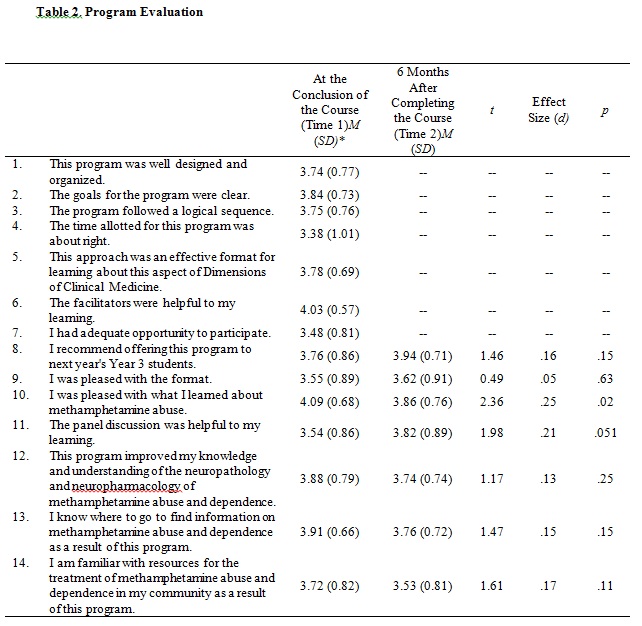
*Mean (Standard Deviation)
Students rated the interclerkship positively and all items were rated above average. Group means for all items were compared between administrations and results are reported in Table 2. Student written comments also provided valuable evaluation data. Many of the comments were general but positive, such as “This was a necessary program for M3 students because most of us have not had exposure to this form of drug abuse. I would highly recommend keeping it with the curriculum next year.” Other student comments noted the value of inviting presenters from the community. For example, one student wrote, “The law enforcement panel did a great job contextualizing the magnitude of methamphetamine use in the community and illustrating the social ramifications of this epidemic in the community.” Several students commented on the value of introducing basic science and clinical content. As one student noted, “I learned more about what to look for in users of this drug that I didn’t know before, and more about pharmacology and social implications of drug abuse.”
The course faculty developed a five-item multiple choice question learning assessment to assess key objectives. Paper copies were distributed at the conclusion of the module (Time 1) and then distributed electronically six months later (Time 2), along with the follow-up program evaluation. These results are demonstrated in Table 3. Although students successfully completed the learning assessment at the conclusion of the course module (Time 1), they demonstrated limited retention of this knowledge six months after the course (Time 2). We were not surprised by this result because the assessment measured recall of discrete facts and statistics unlikely to be addressed during clinical rotations. The learning assessment administered at Time 2 also asked two questions about student use of information presented at the session. When asked “Have you consulted any resources (e.g., NIDA web site) for additional information since the session last September?” 10 students (11.0%) indicated yes and 81 (89.0%) students responded no. However, when asked “Have you used information presented at the Dimensions of Clinical Medicine: Methamphetamine Abuse Program during your clerkship?” almost one-third of the students (n=28, 30.8%) indicated they had used information from the session.
Recommendations for future iterations of this curriculum include extending the 4-hour session to the full-day format to allow more time for an introduction to Motivational Enhancement Therapy (MET), participation of a former methamphetamine-dependent patient in a panel discussion of the treatment process and additional information about community resources.
Table3. Learning Assessment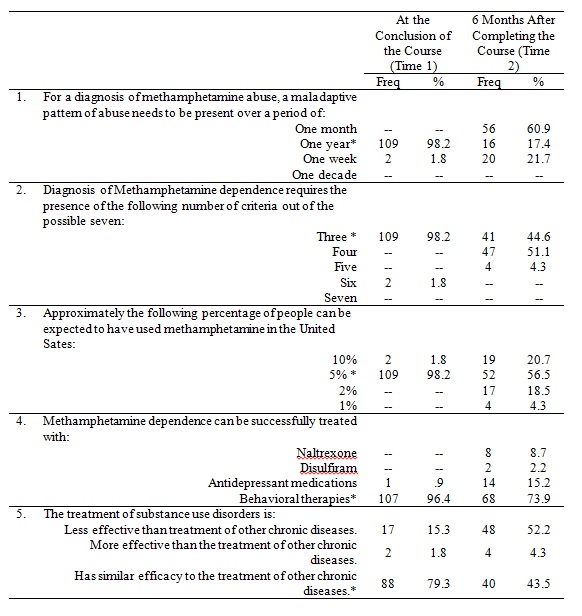
*denotes correct answer
The pilot implementation of the methamphetamine curriculum was successful and the interclerkship format offers a valuable opportunity to teach third-year medical students about an important substance abuse and dependence topic. Including community agency representatives enriched the curriculum and complemented the basic science and clinical content. This curriculum can be easily modified by other medical schools to fit scheduling requirements or even address other substance abuse and dependence topics.
ACKNOWLEDGEMENTS
Funding from the National Institute for Drug Abuse (NIDA) Centers of Excellence for Physician Information program supported the development and evaluation of this curriculum.
REFERENCES
- Griswold, K.S., Aronoff, H., Kernan J.B., and Kahn L.S. Adolescent substance use and abuse: recognition and management. American Family Physician. 2008; 77:331–336.
- Mersy, D.J. Recognition of alcohol and substance abuse. American Family Physician. 2003; 67:1529-1532.
- Fenton, C., Loeser, H., and Cooke M. Intersessions: covering the bases in the clinical year. Academic Medicine. 2002; 77:1159.
- Rest, K.M., Pransky G., and Sweet C. Learning about the environment and health: an interclerkship experience for third-year students. Academic Medicine. 1997; 72:421–422.
- Cardasis, C.A., Hardy S., and Hampl, J. A multidisciplinary interclerkship on hunger and malnutrition. Academic Medicine. 1998; 73:608.
- Jonassen, J.A., Pugnaire, M.P., Mazor, K., Regan, M.B., Jacobson, E.W., Gammon, W., Doepel, D.G., and Cohen, A.J. The effect of a domestic violence interclerkship on the knowledge, attitudes, and skills of third-year medical students. Academic Medicine. 1999; 74:821–828.
- Demmer, L.A., Totzkay, C.M., and Zapka, J.G. An interdisciplinary interclerkship in genetic testing and ethics. Academic Medicine. 2001; 76:538–9.
- Clay, M., Jonassen, J., and Nemitz, A. A one-day interclerkship on end-of-life care. Academic Medicine. 2001; 76:517–518.
- Godkin, M., Ferguson, W., and Diop, D. A required interclerkship on multiculturalism for third-year medical students. Academic Medicine. 2002; 77:469.
- Matthews, J., Kadish, W., Barrett, S.V., Mazor, K., Field, D., and Jonassen, J. The impact of a brief interclerkship about substance abuse on medical students’ skills. Academic Medicine. 2002; 77:419–426.
- Sakowski, H.A., Markert, R.J., Jeffries, W.B., Coleman, R.M., Houghton, B.L., Kosoko-Lasaki, S., Goodman, M.D., and Rich, E.C. Dimensions in clinical medicine: an interclerkship program. Teaching and Learning in Medicine. 2005; 17: 370-375.
- Knowles, M.S. The adult learner. Woburn, MA: Butterworth-Heinemann. 1988.